Diverticular Disease Diet: What to Eat, What to Avoid & How to Prevent Flare-Ups
If you’ve just been diagnosed with diverticular disease, you’re probably feeling a mix of relief and uncertainty.
Relief that it’s nothing more serious.
But also… what now?
What can you actually eat?
Will this get worse?
And how do you stop another flare from happening?”
You might find yourself drowning in advice (not all of it helpful) and even professionals don’t always agree. It’s no wonder it feels confusing.
If you’re sitting there Googling what you can and can’t eat, trying to make sense of it all you’re not alone. Let’s cut through the noise and talk about what actually helps.
What Is Diverticular Disease?
Let’s break down the language first:
- Diverticula are small pouches that can form along the walls of the large intestine.
- Diverticular disease (also known as diverticulosis) is when you have these pouches but no infection.
- Diverticulitis is when those pouches become inflamed or infected.
By age 50, about half of us will have diverticula. By age 80, it’s closer to 70%.
Here is a picture from patient.co.uk that shows what diverticula look like:
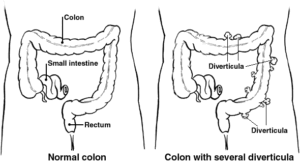
What Causes Diverticular Disease?
What we used to think
Previously it was thought that when there isn’t enough fibre and or fluid, your poo became harder and drier. In turn the movement of your poo through the bowel slows down, increasing pressure in the colon, leading to those little pouches (diverticula) forming.
It was also thought previously that that seeds and nuts irritated the diverticula and that lead to them becoming infected.
What we know now
However, more recent evidence suggests that there maybe a long-term lower grade inflammation in the gut which is the blame. This can be helped by having a wide range of plant based foods in your diet, this in turn helps your gut microbiome produces a range of benefit short chain fatty acids that keep the lining of the gut healthy. Other factors that we know influence gut health such as eating regularly, sleeping well, being active and reducing stress will all help.
If you’re feeling confused or like you’ve somehow caused this, please remember, this is incredibly common and not something you’ve done wrong
Symptoms and Diagnosis of Diverticular Disease
Diverticular disease often mimics IBS:
- Cramping (especially on the left side)
- Bloating
- Diarrhoea or constipation (sometimes both)
A colonoscopy usually confirms the diagnosis.
If you ever notice persistent pain, fever, or blood in your stool, these could be signs of diverticulitis. About 1 in 5 people with diverticular disease will have a flare-up at some point.
What does this diagnosis of diverticular disease actually mean for me long-term?
For most people, diverticular disease is something that can be managed rather than something that takes over your life.
It doesn’t mean you’ll constantly be in pain.
It doesn’t mean you need to cut out large parts of your diet.
In fact, with the right approach, many people find their symptoms settle and become far more predictable. The key is understanding what your body responds to and putting simple, consistent habits in place.
If you’re feeling unsure how this applies to you personally, this is exactly where tailored advice can make a difference
How to Reduce the Risk of Diverticulitis Flare-Ups
- Eat a fibre-rich diet
- Drink 6–8 cups of fluid daily
- Move your body regularly
- Avoid smoking
What Should You Eat with Diverticular Disease?
A high-fibre diet is key. Here’s what that looks like in real life:
Whole Grains
- Wholemeal pasta
- Brown rice
- Oats
- Whole wheat bread
High-Fibre Breakfast Cereals
- Porridge
- Bran flakes
- Weetabix
Beans, pulses, lentils and legumes
Fruit and Vegetables
Aim for at least 5 portions per day. A portion might be:
- 1 medium fruit (e.g. banana, orange)
- 2 small fruits (e.g. plums, satsumas)
- A cereal bowl of leafy greens
- 3 heaped tablespoons of cooked veg or legumes
- A handful of berries or grapes
- A tablespoon of dried fruit

Don’t Skip the fluid
Fibre without fluid is like trying to wash up without water. It won’t work and could actually make constipation worse.
What do I do if a flare of Diverticular disease is starting?
The thought of a flare-up can feel worrying, especially if you’re not sure what it will feel like, or if you’ve experienced one before and are anxious about it happening again.
Many of the people I work with come to me after a flare and say the same thing
they never want to experience that level of pain again. Some describe it as pain that comes in waves, almost like contractions.
If you feel that a flare may be starting, I would always recommend contacting your GP or out-of-hours service for medical advice.
It’s not always easy to tell whether symptoms are a mild flare or something that needs treatment, so it’s important to get the right support early.
While you’re waiting for advice, it can help to keep things simple:
- Stay well hydrated
- Stick to light, regular meals
- Avoid any known trigger foods
If anything feels severe, worsening, or you feel unwell in yourself, seek medical attention promptly.
If you’d like more detailed guidance on what to eat during a flare and how to gradually return to your normal diet, I’ve covered that step-by-step in this article → What to Eat During a Diverticulitis Flare (and When to Change Your Diet)
FAQs: Let’s Bust Some Myths
Can I Eat Nuts and Seeds with Diverticular Disease?
YES. The old advice to avoid them is outdated. They don’t get stuck in diverticula. Constipation is the real issue.
Is Popcorn OK?
YES, just like the myth about seeds and nuts the advice to stop eating popcorn is outdated.
Can I eat Weetabix with diverticular disease?
Yes, Weetabix is fine to have with diverticular disease. If you’re experiencing a flare, you may find lower fibre options like porridge, cornflakes or Rice Krispies easier to tolerate short-term
Should I Avoid Dairy?
Unless you’re also been diagnosed as lactose intolerant (by a health professional), there’s no reason to cut dairy. You’d miss out on valuable nutrients.
Can I Have Spicy Foods?
It depends. Some people tolerate them fine; others don’t. Tune into how your body responds.
You don’t have to keep guessing what to eat with diverticular disease
If you’re feeling confused, stuck, or worried about triggering another flare, you’re not alone. Many of the people I work with felt exactly the same before getting the right support.
Trying to manage this on your own can feel overwhelming, especially when the advice online is so conflicting
With the right approach, it is possible to:
- Feel more confident around food again
- Reduce flare-ups
- Stop second-guessing every meal
If you’ve recently been diagnosed or are struggling to manage your symptoms, this is exactly what I help with.
Book a free 15-minute discovery call and we’ll talk through what’s going on and what your next step could look like.

Fiona Brannigan, BSc (Hons) Human Nutrition & Dietetics, HCPC-Registered Dietitian, Full member of the British Dietetic Association.
Fiona Brannigan is a UK-registered dietitian and founder of Inspirit Nutrition & Dietetic Consultancy, based in Ayrshire and working with clients across the UK. With over 25 years of experience, including more than two decades in the NHS, Fiona has supported thousands of people to improve their health through nutrition.
Her expertise spans gut health, menopause nutrition, digestive disorders, neurological conditions, and rehabilitation following illness. Fiona is particularly passionate about helping adults aged 50+ regain confidence and control over their gut health, manage symptoms such as bloating, constipation, and diarrhoea, and enjoy food without fear or discomfort.
Fiona is regulated by the Health and Care Professions Council (HCPC) and is a member of the British Dietetic Association (BDA). She offers one-to-one consultations online and in person, using evidence-based nutrition and personalised support to help people feel their best at every stage of life.
Book a free discovery call to discuss your gut health goals or learn more about Fiona’s work
Helpful Links and Resources
Trusted External Sites

